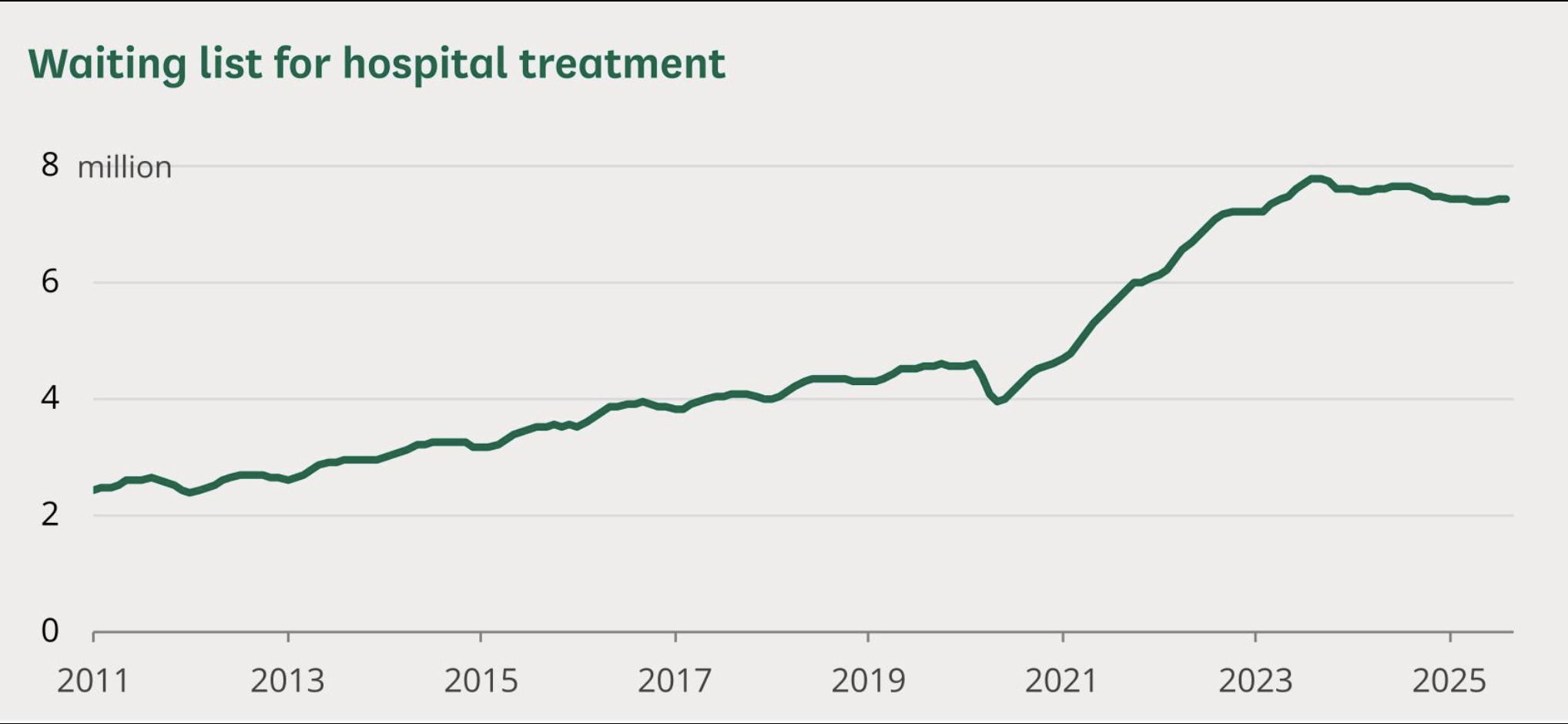
How Ireland Got to 754,000
The accumulation of waiting list numbers in Ireland is not a single event with a single cause. It is the product of a decade of decisions — about capacity, about staffing, about the balance between public and private healthcare, and about what the state was willing to invest — compounded by the pandemic and an accelerating demographic shift that everyone could see coming.
Ireland's population now exceeds 5.3 million, with life expectancy projected at 82.7 years overall in 2025, placing Ireland among the highest in Europe. An ageing, growing population creates predictable demand growth for healthcare. The health service has not kept pace with that demand.
The pandemic's contribution is real but often overstated as an explanatory factor. The trajectory of waiting list growth predates COVID-19. Between 2018 and 2023, scheduled care demand surpassed pre-pandemic levels and demographic expectations — meaning the system was not keeping up even before the additional disruption of 2020 and 2021.
HSE CEO Bernard Gloster offered a framing of the numbers in January 2026 that was designed to provide context without being dismissive: 82% of people who were on waiting lists at the start of January 2025 were not on them at the end of December 2025. That is the throughput of the system — over three-quarters of a million people treated or removed from lists in a single year. The problem is not that the system is not treating people. It is that demand is arriving faster than treatment is occurring, and the people who remain waiting are waiting longer than any target permits.
€420 million was invested in waiting list reduction in 2025. Gloster acknowledged in January that some of this investment — specifically in "third-party insourcing," the practice of sending public patients to private facilities for treatment at public expense — was "not an appropriate or sustainable use of that money" and that the approach is being changed in 2026.
What the Targets Actually Said — and What Was Missed
The 2025 Waiting List Action Plan set four headline targets. None were met:
50% of patients within Sláintecare wait times. The December 2025 figure was 36%. The target was 50%. Fourteen percentage points is not a minor shortfall.
90% of outpatients waiting less than 12 months. Outpatient appointment waiting lists grew through most of 2025. The specific figure against this target was not disclosed at the time of reporting, but the overall trajectory was in the wrong direction.
Waiting list volume reduction. The total number on lists increased by 86,300 during 2025 — a net increase despite record levels of investment and activity.
Long-waiter reduction. Here the system made measurable progress. The number of patients waiting over twelve months fell by approximately 55% — or 155,000 fewer long-waiters — since September 2021 when the multi-annual action plan began. The number waiting eighteen months or more fell significantly. 7,540 adults and 510 children are currently waiting eighteen months or more — still a breach of Sláintecare targets, but substantially lower than the equivalent figure four years ago.
The pattern that emerges from these numbers is consistent: the system has made real progress at the extreme end — the longest-waiters — while struggling to manage overall volume and to convert the majority of new patients into timely appointments.
The WTAP 2026 and What It Promises
The Waiting Time Action Plan 2026 was published by Minister for Health Jennifer Carroll MacNeill in January. It sets 36 actions under three themes: Reforming Planned Care, Enabling Planned Care, and Capacity Optimisation.
The headline targets for 2026:
- 50% of patients to be waiting less than Sláintecare wait times of ten weeks for outpatient appointments and twelve weeks for inpatient procedures
- 90% of patients to be waiting less than twelve months for outpatient services
- Weighted average wait time below 5.5 months for outpatient and inpatient procedures
These are the same headline targets that were missed in 2025. The government is setting them again because missing a target does not make it wrong to pursue it — but it does raise the question of what changes in 2026 that would produce a different result.
The plan points to several specific initiatives. An OPD Clinic Capacity Optimisation Programme piloted across four hospitals in 2025 generated an estimated additional 2,700 new outpatient appointments — the programme will be expanded in 2026 with a projected 103,000 additional OPD attendances. Artificial intelligence and automation are being deployed to improve waiting list management. An endoscopy reporting system and electronic referral system are being extended. Centralised referrals and pooled waiting lists — where patients are assigned to the next available consultant rather than waiting for their specific referring consultant — are being introduced.
Carroll MacNeill is also introducing a formal oversight structure that was not present in previous action plans: a Waiting List Task Force co-chaired by the Department of Health Secretary General and the HSE CEO, reporting directly to the Minister. This is an accountability mechanism as much as a management mechanism — it creates a named structure responsible for delivery, rather than distributing responsibility diffusely across the system.
The Regional Dimension
One of the persistent features of Irish healthcare waiting times is that they vary enormously by region and by specialty. The HSE acknowledged in the National Service Plan 2026 that some areas have patients seen quickly while others face severe backlogs "even in health regions that perform well in other areas." Community therapies — speech and language, occupational therapy, physiotherapy — face severe backlogs across most of the country regardless of how their regional acute hospital performs.
The establishment of six Health Regions and twenty Integrated Health Areas under Sláintecare is designed to address this by enabling population-focused planning — aligning resources with local need rather than managing services from a single national structure. 2026 is described as "the first major step" toward this model. The implication is that the benefits of regional restructuring are not yet visible in waiting list data and will take time to materialise.
The practical effect for patients is that where you live in Ireland continues to determine your healthcare experience in ways that the stated policy commitment to universal access explicitly rejects. A patient in a well-resourced urban Health Region with high consultant density faces a different wait time than a patient in a rural region relying on outreach services. The WTAP 2026 acknowledges this explicitly: "wherever you live in Ireland, you should have timely access to high-quality care." The data shows the gap between that commitment and the current reality.
What None of This Is About
It is worth being specific about what the waiting list problem in Ireland is not.
It is not primarily a funding problem in the simple sense that more money would immediately resolve it. €420 million was invested in 2025 with results that were real in some areas and absent in others. The constraint is structural — consultant capacity, theatre availability, primary care services that could absorb demand before it reaches hospitals — and structural constraints are not resolved by a single year's investment.
It is not a problem that can be solved by restructuring alone. The Sláintecare reform architecture — Health Regions, Integrated Health Areas, population-based funding — is a necessary set of changes. But restructuring does not immediately treat patients. The transition costs of reorganisation are real, and the benefits are medium-term.
And it is not a problem that affects everyone equally. Private health insurance — held by approximately 45% of the Irish population — provides access to private hospitals and consultants that substantially reduces waiting times for those who can afford it. The two-tier system that Sláintecare was designed to end remains the operational reality. The 754,000 people on public waiting lists are, overwhelmingly, the people without private insurance.
That is the context in which the Waiting Time Action Plan 2026 sits. The targets are correct. The direction is correct. The question every year is whether the system can actually move faster than demand grows — and in 2025, it could not.
